Governmental action (or inaction) that affects America at large often has an outsized impact on rural residents.
At the end of February, the Trump administration announced it will withhold millions of dollars in Medicaid reimbursements to Minnesota, citing concerns about fraud. This comes on the heels of GOP cuts to Medicaid in the 2025 budget reconciliation bill and an effort to repeal the Affordable Care Act (ACA), which would disproportionately hurt rural healthcare systems.
The Daily Yonder explains how rural inequality manifests in this scenario: Rural hospitals are more likely than urban hospitals to operate with negative profit margins. And cuts to public payer programs, like Medicare or Medicaid, disproportionately threaten these hospitals by increasing the rate of uncompensated care, or services for which hospitals receive no payment.
The following map shows the percentage of revenue in rural hospitals that comes from federal and state-level health insurance programs for low-income families.
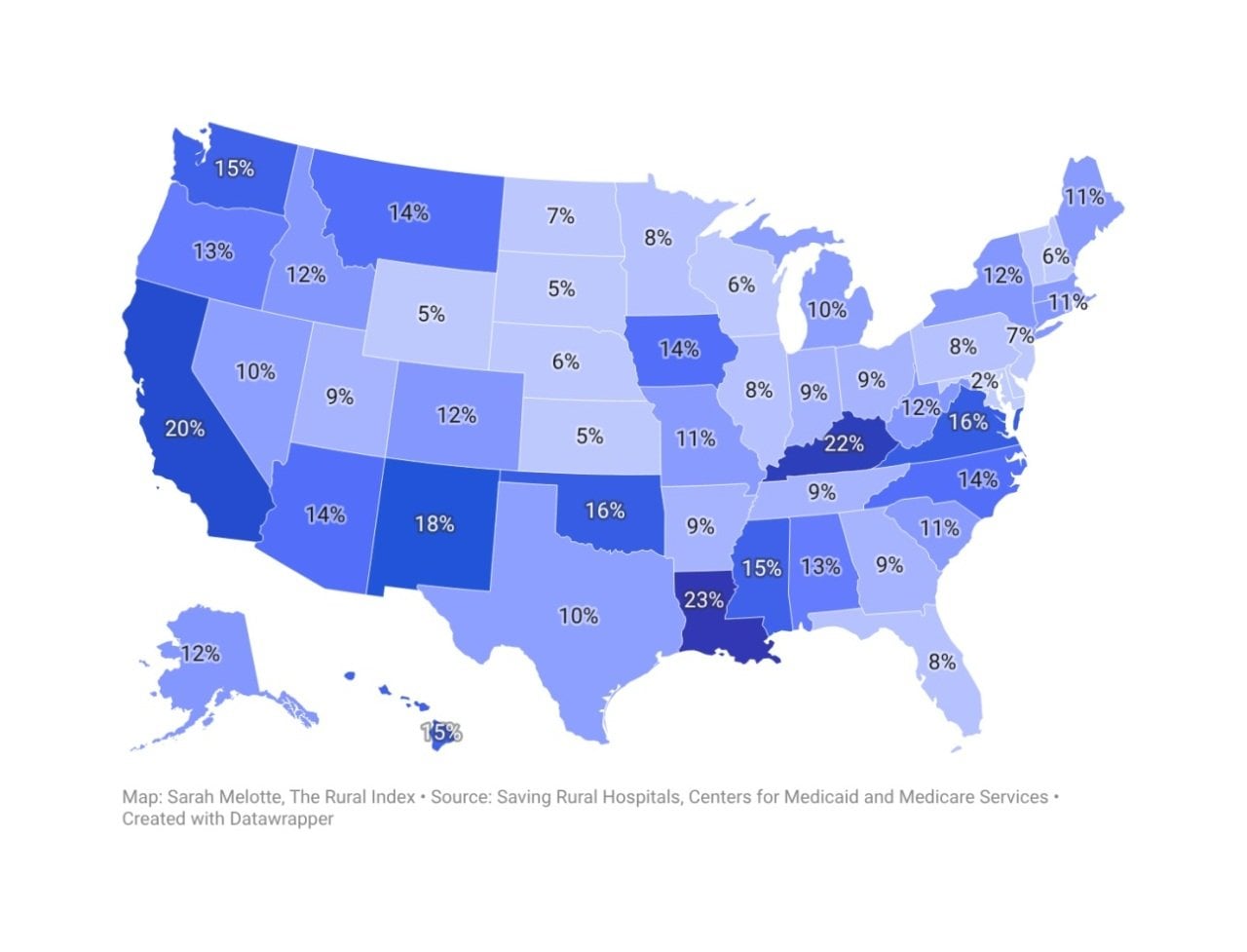
All hospitals receive reimbursements from programs like Medicaid, CHIP, or state-level health insurance programs. In rural hospitals, Medicaid accounts for about 19% of discharges. But that share varies from hospital to hospital, depending in part on how much of the surrounding population relies on public insurance.
Keep in mind that this map does not reflect payer mix, or the share of the total population that receives governmental health insurance assistance for low-income families. It only shows the share of revenue derived from low-income assistance programs, which is not directly proportional to the share of patients on those programs.
Data for this analysis comes from Saving Rural Hospitals, a website created by the Center for Healthcare Quality and Payment Reform, a national policy organization that advocates for improvements in healthcare systems.
In a Feb. 25 press conference at the White House, CMS Administrator Mehmet Oz announced that the Trump administration plans to withhold $259 million from Minnesota’s Medicaid program. Oz claimed that money allotted for low-income families went to bogus organizations and a behavioral health clinic that paid doctors to work 24 hours a day for more than 450 days.
In a statement on X, Minnesota Gov. Tim Walz criticized the agency’s method of combating fraud, stating that the Trump administration is on a “campaign of retribution,” and that Medicaid cuts would be “devastating” for working families across the state. “The agents Trump allegedly sent to investigate fraud are shooting protesters and arresting children,” Walz said.
Minnesota Attorney General Keith Ellison called the Trump administration’s plans unlawful, threatening to take them to court if they continued to withhold Medicaid funds.
Accessible Space, a Minnesota nonprofit that offers affordable housing to people with disabilities, is funded almost entirely through Medicaid reimbursements. Director of Accessible Space Josh Berg told Minnesota Public Radio that “any cuts to Medicaid funding will directly result in reduced services.”
And many rural hospitals in Minnesota — and across rural America at large — face similar circumstances. Thirty-nine of Minnesota’s 98 rural hospitals have negative operating margins, according to Daily Yonder analysis of CMS data.
Some hospitals with persistently negative operating margins manage to stay afloat by relying on nonoperating revenue, or revenue that comes from sources like taxes and philanthropy. But even that cushion isn’t always enough. More than 100 rural hospitals have closed in the United States in the last decade alone, forcing rural families to travel further to get the care they need.
Trump’s campaign against supposed fraud isn’t an abstract war in rural Minnesota. In communities where hospitals operate on thin margins, even small cuts in federal spending can destabilize entire systems of care.
This story was produced by The Daily Yonder and reviewed and distributed by Stacker.
Reader Comments(0)